 By Michael E. Ash BSc DO ND and Garth L. Nicolson, PhD
By Michael E. Ash BSc DO ND and Garth L. Nicolson, PhD
On the front line of primary care the two most common complaints are fatigue and gastrointestinal problems. Fatigue is the most common; up to 45% of consultations mention fatigue as the major complaint.[1],[2] If unresolved, it can progress to the point that it causes disability comparable to that found in chronic medical patients.[3],[4] Most people suffering from fatigue do not initially seek primary care intervention but self-treat with stimulants such as caffeine, herbs, tonics and sugars. Although these can provide short-term increases in energy and perception of reduced fatigue, they have potential long-term adverse health effects. [5],[6]
Common disorders of the gastrointestinal (GI) tract account for about 50 million visits per year to physicians trained in traditional allopathic or osteopathic medicine.[7] This amounts to 30% to 50% of all people with persistent abdominal symptoms who seek help once their own experimentation with food selection and over the counter medications has been exhausted. Just as with patients complaining of fatigue, it is a loss of quality of life that most frustrates them. [8],[9] Their symptoms might be an expression of a physical illness (e.g., Crohn’s disease), a mental illness (e.g., panic disorder), and/or a functional disorder. About half of all adults who consult a primary care physician or gastroenterologist because of chronic abdominal discomfort for more than three months are ultimately diagnosed as having a functional bowel disorder. Loss of health-supporting GI bacterial symbiosis, a state known as dysbiosis, represents a primary trigger in both functional and pathological disorders of the digestive tract. Studies have demonstrated that intestinal dysbiosis, characterized mainly by altered bacterial composition and loss of diversity, is strongly associated with the development of gut dysfunction.[10] We will explain the molecular connection between fatigue and dysbiosis that pivots around mitochondrial health and discuss current evidence for membrane related treatments using lipid replacement therapy (LRT®).
The integrity of mitochondrial membranes is critical to cell function and energy metabolism. This membrane is the frontier between cell survival and death.
Overview of Fatigue
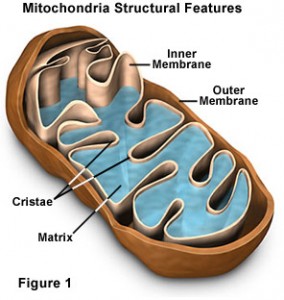
Just as many roads lead to Rome, many conditions lead to fatigue. But at the core is mitochondrial dysfunction. The mitochondria are the energy powerhouses of our cells. And the mitochondria cannot function, or cannot generate energy through electron transport, without healthy and intact membranes. The integrity of mitochondrial membranes is critical to cell function and energy metabolism.
Fatigue begins and ends with the mitochondrial membrane. Guido Kroemer, M.D., Ph.D., a French scientist known for his groundbreaking work on the mitochondrial membrane, has called this membrane the “battleground on which opposing signals combat to seal the cell’s fate…the frontier between survival and death.”[11] His discovery that mitochondria control cell death was considered revolutionary, and it has shaped much subsequent research.
In healthy cells, the inner mitochondrial membrane where the electron transport system is located is nearly impermeable, and this is important in establishing inner membrane trans-membrane chemical/electrical potential essential for oxidative phosphorylation. When a cell begins to die, it is in large part due to disrupted, damaged, increasingly permeable mitochondrial membranes. Permeability of the mitochondrial membranes constitutes a point-of-no-return in programmed cell death. Importantly, mitochondria are responsible for production of most of our cell’s reactive oxygen species (ROS) and some reactive nitrogen species (RNS). Significant oxidative damage to mitochondrial membranes represents the point-of-no-return of programmed cell death pathways that culminate in apoptosis or regulated cell death leading to necrosis.[12]
Mitochondrial membrane permeability is affected in ischemia, viral and bacterial infections, metabolic diseases, neurobehavioral and neurodegenerative diseases, among other disorders, according to Kroemer and colleagues. For example, viral proteins can induce mitochondrial membrane permeability, followed by swelling and fragmentation.11 It appears that chronic neurodegenerative diseases, such as Alzheimer’s, amyotrophic lateral sclerosis, Huntington’s and Parkinson’s disease, may also involve mitochondrial dysfunction and increases in mitochondrial permeability. Many other conditions, such as heart disease, metabolic syndrome, dysbiosis related illnesses and even psychiatric conditions have been linked to loss of mitochondrial membrane function and increases in membrane permeability.
How Damaged Mitochondria Wreak Havoc
Damage to mitochondrial components, especially the delicate inner mitochondrial membrane, leads to the release of toxic proteins, including caspases and other enzymes. These proteins are normally confined in the mitochondria, but once released these proteins go through several steps that trigger the formation of a potent inflammatory molecular complex called an inflammasome. New evidence has placed inflammasomes at the center stage of complex diseases like metabolic syndrome and cancer, as well as the regulation of the microbial ecology in the intestine and the production of ATP.[13],[14],[15],[16],[17],[18],[19] Inflammasomes are regarded by some scientists as ‘guardians of the body’ because of the way they orchestrate host defenses and their role in the pathogenesis of inflammatory diseases.[20]
Lipid replacement therapy (LRT)® that emulates the amount and composition of the mitochondrial lipids assures that mitochondrial membrane permeability is maintained in the optimal range
Once the inner membrane of the mitochondria is damaged, its core ability to produce energy in the form of ATP and to maintain optimal mitochondrial nutrient uptake and utilization necessary for ATP production are impaired. The result is perceived as persistent fatigue.
Mitochondria are also responsible for many metabolic circuits and signaling pathways. Just a few examples of these include: oxidative phosphorylation; biosynthesis of key molecules, including heme and certain steroids as well as in many catabolic energy relevant pathways, such as the β-oxidation of fatty acids; and regulation of calcium homeostasis.[21]
In addition, the immune system is stimulated by molecular byproducts of mitochondrial damage to produce inflammatory cytokines. If inappropriately regulated, these cytokines then sustain and even promote local and systemic inflammation in a ‘feed-forward’ cycle of inflammatory messengers. Once the mucosal innate immune system is switched on to high-alert by the inflammasome, GI bacteria become involved in this process, and the local specialized sensors become hyper-responsive to bacterial triggers from the gastrointestinal tract – even from previously tolerated bacteria. This leads to loss of mucosal barrier integrity in the gut, dysbiosis, inflammation and fatigue. [22],[23] More inflammasomes are then produced, leading to a vicious cycle and chronic tissue damage.
How to Restore the Mitochondrial Membrane
The mitochondrial membrane contains the major classes of phospholipids found in all cell membranes, including phosphatidylcholine (PC), phosphatidylethanolamine (PE), phosphatidylinositol (PI), phosphatidylserine
(PS), and phosphatidic acid (PA), as well as phosphatidylglycerol
(PG), the precursor for cardiolipin (CL); which is predominantly located in the mitochondria.
Using lipid replacement therapy (LRT®) in the form of a stable oral supplement that emulates the amount and composition of the mitochondrial lipids assures that inappropriate oxidative membrane damage is prevented, damaged membrane phospholipids are replaced and mitochondrial membrane permeability is maintained in the optimal range. It also reduces the number of mitochondrial DNA deletions. Thus LRT® can be used to restore mitochondrial and other cellular membrane functions via delivery of undamaged replacement lipids to cells and that, in turn, can reduce inflammasome promotion.
Recent clinical trials using patients with chronic fatigue or chronic fatigue syndrome[24] have shown the benefit of LRT®. Using naturally occurring membrane phosphatidyl lipids listed above, mitochondrial electron transport function can be restored and moderate to severe chronic fatigue can be significantly reduced in the process. [25]
Additional studies have also identified significant improvements in energy, mood, affect and function in a healthy population following ingestion of the glycophospholipids in a drink. [26],[27]
In one impressive study LRT® reduced fatigue 35.5% in aging adults and significantly improved mitochondrial function to a level that was similar to that found in young, healthy adults
In recent studies, LRT and B Vitamins given for 6 months or more has also reduced the blood levels of the amino acid homocysteine, which are related to increased risk for cardiovascular disease, stroke, cognitive loss, depression and immune dysfunction. [28]
The use of LRT® is attractive as a safe and effective intervention in the treatment of persistent and transient fatigue. Studies have been conducted on various populations, from those with normal health and function to those undergoing complex treatments for cancer and those with persistent fatigue. These groups have shown between 30-45% improvement in fatigue perception and function 25,26,27 utilizing the internationally recognized Piper Fatigue Scale. [29] In addition, in concert with significant fatigue reduction, a cross-over clinical trial has shown that mitochondrial function was also significantly improved. [30] Even in severely fatigued patients with chronic fatigue syndrome or fibromyalgia syndrome, LRT® reduced fatigue by 43.1%.25
In one impressive study LRT® reduced fatigue 35.5% in aging adults and significantly improved mitochondrial function to a level that was similar to that found in young, healthy adults. 30
Mitochondria, the Gut and Immune Regulation: An Evolving Comprehension
As indicated, recent studies suggest that mitochondria are significant players in the orchestration of innate immune responses via the inflammasome, which results in the production and release of the pro-inflammatory cytokines IL-1β and IL-18.[31],[32] These, in turn, contribute to the symbiosis/dysbiosis of the bacterial organisms that reside in our digestive tract. The digestive tract is home to trillions of bacteria, and is also the site of greatest density of innate immune receptors in the body. These receptors are key mediators in the management and maintenance of immune responses and tolerance, and play a role in determining bacterial composition.[33] Their inappropriate activation and their expression mediated by IL-1β and IL-18 leads to altered innate immune receptor hyper-responsiveness and may contribute to immune-mediated inflammatory diseases as well as fatigue via inflammasomes that induce dysbiosis.[34]
Thus it’s likely that mitochondrial damage creates fatigue not only directly by impairing mitochondrial function, but also indirectly through pro-inflammatory promotion of cytokines and inflammasomes, the consequences of which include local inflammation, loss of mucosal barrier integrity, dysbiosis and fatigue. [35],[36] A cautiously optimistic idea is now taking hold that invokes using mitochondrial-induced symbiosis of the gut microbiota to track, target and treat a plethora of diseases, even ones beyond the confines of the gastrointestinal tract.[37]
This sequence of events places mitochondria at the cross roads of bioenergetics, cell death signaling, microbial ecology and the innate and adaptive immune system, and associated inflammation.
Inflammation is, of course, an essential immune response that enables survival during infection or injury and maintains tissue homeostasis under a variety of noxious conditions. Inflammation comes at the cost of a transient decline in local tissue function, which in turn contributes to the pathogenesis of diseases and loss of function related to altered homeostasis. Inflammation, at least at the molecular level, has been described as the ‘common soil’ of altered health and function.[38]
Lipid Replacement: An Ideal Approach?
Pro-inflammatory cytokines are capable of inducing many if not all the cardinal symptoms of CFS in humans. [39],[40] The use of LRT® is attractive, since it can restore mitochondrial membranes and the gut milieu, including its delicate lining at the same time. The resolution of inflammasome-induced dysbiosis makes a considerable contribution towards improving mitochondrial fitness; just as mitochondrial fitness contributes to the management of healthy, gut-mediated immune reactivity and associated symbiosis.
The results of using LRT® and the subsequent recovery from fatigue provided by LRT® are consistent and profound.25,26,27,28,30
This health altering intersection of immunity, inflammasome activation, oxidative stress and dysbiosis, can be found in the membranes of the mitochondria residing in our cells – not only of the gastrointestinal tract but all other tissues as well.
The clinical use of LRT® has the potential to decrease the adverse effects of aging on mitochondria and improve mitochondrial function in various chronic diseases, diminish fatigue and improve altered states of mucosal immunity and associated microbial ecology through the participatory resolution of inflammasome-mediated dysbiosis. The improvement in terms of restitution of mucosal and immunological tolerance has potential health benefits that extend systemically..[41],
In summary, LRT® is not just the dietary substitution of lipids with proposed health benefits; it is the actual replacement of damaged cellular lipids with undamaged lipids to ensure proper structure and function of cellular structures, mainly cellular and organelle membranes that contribute to important functional support of good health.25,30
References
[1] Lewis G, Wessely S: The epidemiology of fatigue: more questions than answers. J Epidemiol Community Health 1992; 46(2):92-97. View Full Paper
[2] Cloninger CR. A systematic method for clinical description and classification of personality variants. A proposal. Arch Gen Psychiatry. 1987;44(6):573-588. View Abstract
[3] Nelson E, Kirk J, McHugo G, Douglass R, Ohler J, Wasson J, Zubkoff M. Chief complaint fatigue: a longitudinal study from the patient’s perspective. Fam Pract Res J. 1987;6(4):175-188. View Abstract
[4] Nijrolder I, van der Windt DA, van der Horst HE. Prognosis of fatigue and functioning in primary care: a 1-year follow-up study. Ann Fam Med. 2008;6(6):519-527. View Abstract
[5] Gunja N, Brown JA. Energy drinks: health risks and toxicity. Med J Aust. 2012;196(1):46-49. View Abstract
[6] Arria AM, Caldeira KM, Kasperski SJ, Vincent KB, Griffiths RR, O’Grady KE. Energy drink consumption and increased risk for alcohol dependence. Alcohol Clin Exp Res. 2011;35(2):365-375. doi: 10.1111/j.1530-0277.2010.01352.x. Epub 2010. View Abstract
[7] Michelfelder AJ, Lee KC, Bading EM. Integrative medicine and gastrointestinal disease. Prim Care. 2010 ;37(2):255-267. Review. View Abstract
[8] Wilson S, Roberts L, Roalfe A, Bridge P, Singh S. Prevalence of irritable bowel syndrome: a community survey. Br J Gen Pract. 2004;54(504):495-502. View Abstract
[9] Oberndorff-Klein Woolthuis AH, Brummer RJ, de Wit NJ, Muris JW, Stockbrügger RW. Irritable bowel syndrome in general practice: an overview. Scand J Gastroenterol Suppl. 2004;241:17-22. . View Abstract
[10] Ott SJ, Musfeldt M, Wenderoth DF, Hampe J, Brant O, Fölsch UR, Timmis KN, Schreiber S.Reduction in diversity of the colonic mucosa associated bacterial microflora in patients with active inflammatory bowel disease. Gut. 2004;53(5):685-693. View Abstract
[11] Kroemer G, Galluzzi L, Brenner C. Mitochondrial Membrane Permeabilization in Cell Death. Physiol Rev. 2007;87:99–163. View Full Paper
[12] Nakahira K, Haspel JA, Rathinam VA, Lee SJ, Dolinay T, Lam HC, Englert JA, Rabinovitch M, Cernadas M, Kim HP, Fitzgerald KA, Ryter SW, Choi AM. Autophagy proteins regulate innate immune responses by inhibiting the release of mitochondrial DNA mediated by the NALP3 inflammasome. Nat Immunol. 2011;12(3):222-2230. Epub 2010 Dec 12. View Abstract
[13] Franchi L, Muñoz-Planillo R, Núñez G. Sensing and reacting to microbes through the inflammasomes. Nat Immunol. 2012;13(4):325-332. doi: 10.1038/ni.2231. View Abstract
[14] Chen GY, Núñez G. Inflammasomes in intestinal inflammation and cancer. Gastroenterology. 2011;141(6):1986-1699. Epub 2011 Oct 15. View Abstract
[15] Stienstra R, van Diepen JA, Tack CJ, Zaki MH, van de Veerdonk FL, Perera D, Neale GA, Hooiveld GJ, Hijmans A, Vroegrijk I, van den Berg S, Romijn J, Rensen PC, Joosten LA, Netea MG, Kanneganti TD. Inflammasome is a central player in the induction of obesity and insulin resistance. Proc Natl Acad Sci U S A. 2011;108(37):15324-15329. Epub 2011 Aug 29. View Abstract
[16] Bansal AS, Bradley AS, Bishop KN, Kiani-Alikhan S, Ford B. Chronic fatigue syndrome, the immune system and viral infection. Brain Behav Immun. 2012;26(1):24-31. Epub 2011 Jul 2.. View Abstract
[17] Maes M, Twisk FN, Kubera M, Ringel K. Evidence for inflammation and activation of cell-mediated immunity in Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS): increased interleukin-1, tumor necrosis factor-α, PMN-elastase, lysozyme and neopterin. J Affect Disord. 2012;136(3):933-939. Epub 2011 Oct 4. View Abstract
[18] Franklin BS, Latz E. For gut’s sake: NLRC4 inflammasomes distinguish friend from foe. Nat Immunol. 2012;13(5):429-431. doi: 10.1038/ni.2289. View Abstract
[19] Henao-Mejia J, Elinav E, Jin C, Hao L, Mehal WZ, Strowig T, Thaiss CA, Kau AL, Eisenbarth SC, Jurczak MJ, Camporez JP, Shulman GI, Gordon JI, Hoffman HM, Flavell RA. Inflammasome-mediated dysbiosis regulates progression of NAFLD and obesity. Nature. 2012;482(7384):179-185. doi: 10.1038/nature10809. View Abstract
[20] Martinon F, Mayor A, Tschopp J. The inflammasomes: guardians of the body. Annu Rev Immunol. 2009;27:229-265. . View Abstract
[21] Kroemer G, Galluzzi L, Brenner C. Mitochondrial membrane permeabilization in cell death. Physiol Rev. 2007;87(1):99-163.. View Abstract
[22] Maes M. Inflammatory and oxidative and nitrosative stress pathways underpinning chronic fatigue, somatization and psychosomatic symptoms. Curr Opin Psychiatry. 2009;22(1):75-83. View Abstract
[23] Kelly D, Delday MI, Mulder I. Microbes and microbial effector molecules in treatment of inflammatory disorders. Immunol Rev. 2012;245(1):27-44. . View Abstract
[24] Avellaneda Fernández A, Pérez Martín A, Izquierdo Martínez M, Arruti Bustillo M, Barbado Hernández FJ, de la Cruz Labrado J, Díaz-Delgado Peñas R, Gutiérrez Rivas E, Palacín Delgado C, Rivera Redondo J, Ramón Giménez JR. Chronic fatigue syndrome: aetiology, diagnosis and treatment. BMC Psychiatry. 2009 Oct 23;9 Suppl 1:S1. Review. View Abstract
[25] Nicolson, G.L. and Ellithrope, R. Lipid replacement and antioxidant nutritional therapy for restoring mitochondrial function and reducing fatigue in chronic fatigue syndrome and other fatiguing illnesses. J. Chronic Fatigue Syndr. 2006;13(1): 57-68. View Full Paper
[26] Ellithorpe RA, Settineri R, Mitchell CA, Jacques B, Ellithorpe E, Nicolson GL. Lipid replacement therapy drink containing a glycophospholipid formulation rapidly and significantly reduces fatigue while improving energy and mental clarity. Funct Food Health Dis. 2011;1(8): 245-254. View Full Paper
[27] Nicolson GL, Ellithorpe RR, Ayson-Mitchell C, Jacques B, Settineri R. Lipid Replacement Therapy with a Glycophospholipid-Antioxidant-Vitamin Formulation Significantly Reduces Fatigue Within One Week. J Am Nutraceut Assoc. 2010;13(1):10-14 View Full Paper
[28] Nicolson GL, Ellithorpe R and Settineri R. Blood homocysteine levels are significantly reduced with a glycophospholipid formulation (NTFactor® plus vitamin B-complex): a retrospective study in older subjects. Paper in Preparation.
[29] Piper BF, Dibble SL, Dodd MJ, Weiss MC, Slaughter RE, Paul SM. The revised Piper Fatigue Scale: psychometric evaluation in women with breast cancer. Oncol Nurs Forum. 1998;25(4):677-684. View Abstract
[30] Agadjanyan M, Vasilevko V, Ghochikyan A, Berns P, Kesslak P, Settineri R, Nicolson GL. Nutritional supplement (NTFactor) restores mitochondrial function and reduces moderately severe fatigue in aged subjects. J Chronic Fatigue Syndr 2003;11(3):23-26. View Full Paper
[31] Tschopp J. Mitochondria: Sovereign of inflammation? Eur J Immunol. 2011;41(5):1196-1202. doi: 10.1002/eji.201141436. . View Abstract
[32] Franchi L, Muñoz-Planillo R, Núñez G. Sensing and reacting to microbes through the inflammasomes. Nat Immunol. 2012;13(4):325-332. doi: 10.1038/ni.2231. View Abstract
[33] Rakoff-Nahoum S, Paglino J, Eslami-Varzaneh F, Edberg S, Medzhitov R. Recognition of commensal microflora by toll-like receptors is required for intestinal homeostasis.Cell. 2004;118(2):229-241. View Abstract
[34] Lakhan SE, Kirchgessner A. Gut inflammation in chronic fatigue syndrome. Nutr Metab (Lond). 2010;7:79. View Abstract
[35] Circu ML, Aw TY. Intestinal redox biology and oxidative stress. Semin Cell Dev Biol. 2012; Mar 30. [Epub ahead of print] View Abstract
[36] Maes M. Inflammatory and oxidative and nitrosative stress pathways underpinning chronic fatigue, somatization and psychosomatic symptoms. Curr Opin Psychiatry. 2009;22(1):75-83. . View Abstract
[37] Korecka A, Arulampalam V. The gut microbiome: scourge, sentinel or spectator? J Oral Microbiol. 2012;4. doi: 10.3402/jom.v4i0.9367. Epub 2012 Feb 21. View Abstract
[38] Scrivo R, Vasile M, Bartosiewicz I, Valesini G. Inflammation as “common soil” of the multifactorial diseases. Autoimmun Rev. 2011;10(7):369-374. Epub 2010 Dec 30. Review. View Abstract
[39] Dantzer R, O’Connor JC, Freund GG, Johnson RW, Kelley KW: From inflammation to sickness and depression: when the immune system subjugates the brain. Nat Rev Neurosci. 2008;9:46-56. View Abstract
[40] Raison CL, Lin JM, Reeves WC: Association of peripheral inflammatory markers with chronic fatigue in a population-based sample. Brain Behav Immun. 2009;23:327-337. View Abstract
[41] Wu HJ, Wu E. The role of gut microbiota in immune homeostasis and autoimmunity. Gut Microbes. 2012 ;3(1). [Epub ahead of print] View Abstract





14 Comments. Leave new
Your paper was most informative and extremely interesting. I have a particular interest in a number of conditions and their relationship to gut flora. I am a registerd Craniosacral Therapist and as a dicipline this is relient upon membranes throughout the body performing not only a communication role, but also a medium for healing. Dysfunction within the membranes results in many conditions arising as a result of blockages within this system. Blockages being responsible for trauma to the healthy functioning / homeostasis within the myriad of bodily systems. It is very often the removal of these blockages within the membranes that results in the resolution of the specific condition. It is also the case that most conditions are multifactorial in origin, and this is helped by the practisioner holding a neutral space for their clent through which the various component challenges are allowed to express themselves to a resolution.
Your discussion of the role of mitochondria is and membrane trauma is therefore of particular interest and I look forward to hearing more in the up coming conference.
Hi Jack
Thank you for your feedback and I look forward to seeing you at the upcoming conference. I hope you will encourage your colleagues to attend also.
One of the quotes I like in terms of mitochondria is:
Obviously when discussing mitochondrial membrane functionality it can become very complex – molecular medicine is a very intense area of investigation, and the 1500 genes of our mitochondria are poorly understood in terms of their impact on health. However, the interpaly between multiple organisms and multiple signalling pathways seem to find their way back to our mitochondrial function. Reduction of inappropriate ROS and diminished inappropriate autophagy and membrane competence make for exciting times in clinical medicine.
Prof Nicolson is a world leader in membrane physiology and it will be very interesting for all of us to discover how our preferred route of health mediation may influence mitochondrial functionality and equally how we may use glycophospholipids to hasten this.
Hi Michael,
That’s a very interesting paper, thank you. Could intracellular permeability in the gut indicated by raised Mannitol levels in a permeability test be reversed with Lipid Replacement Therapy? I know it would be important to remove trigger first etc. Would I be right in saying that although glutamine may be helpful in treating intercellular permeability, it is less effective in treating intracellular?
Hi Melissa
You may be correct – the epithelial tissues of the gut are highly dynamic and rapid in their pace of replacement, the use of glycophospholipids to repair the trans and paracellular functionality of the gut may well be managed through lipid restoration, as will the removal of promoter agents and supply of food substrates including glutamine and epithelial growth factor.
Michael,
I received a brochure in the mail called In Focus – NutriCology Newsletter where they talked about LRT so I decided to search the internet and found your article. I have been disgnosed with osteoarthritis – both hips have been replaced. Now, at 57, I need ankle replacement and shoulder replacement on one side – needless to say the other side is showing the same symptoms. Would this help me and how can I get it? This sound like something that could work for me, although no doctor has suggested it.
Thank you.
Hi Mary
Thank you for your inquiry. LRT is a fascinating complex of cell specific lipids that enhance the membrane health of cells and the inner mitochondria. These are important components of human physiology, but I regret that the use of LRT for the management of degenerative joints is unlikely to be significantly beneficial. If as a result of the destructive consequences you have fatigue, but the pain is managed, it may offer you increased functionality.
The product Arthred, a collagen complex may be a better option, as this has undergone human trials for the management of osteo-arthritis and most subjects were able to significantly reduce their need for painkillers or discontinue them after 3 months treatment.
Best wishes
Michael
Where can one find LRT supplements?
In the USA – Allergy Research Group provide a range of products that contain LRT
Would lipid replacement therapy , as a functional food, have a role to play in healing gut membrane for anyone taking antiretroviral ‘therapy’ for a diagnosis/classification of HIV. Reading around on gut dysbiosis mitochondrial damage oxidative stress anerobic dysfunction and apoptosis etcetc it seems to me there is a huge lack in treatment options for us. I am diagnosed /classified as HIV Positive and struggling with the toxicity . I feel my gut has been destroyed and in recent years I have refused all extras – like vaccinations for flu – to try to limit additional pathogenic trauma. I have read about HEP B contamination and so on , Not keen to continue treatment unless I can complement with some supportive therapy to counter the toxicity and provide nutritional therapy . I believe they have a role to play in healing our bodies and also in optimising the role chemo might at times have to play . Have you any suggestions on this – in context of supportive treatments . Not a drug user , dont drink alcohol or smoke . Experience huge energy crashes low white counts and pain indicative of neutrophil plummets – lower back, chest , neck , chills , fatigue , slurred speech. It lasts days to one two weeks and then passes with complete rest . I have had this for years prior to diagnosis from teens . Lots of infections as a child. Eye, chest respiratory . Mononuc. + , CMV + from childhood. Cats , Dogs , Rabbits Horses as pets. Strange viral infection at 20 with yellow projectile nausea – but it affected most of street at the time. Hep B vaccinations causing progressive drop in CD4 , fatigue and weight loss followed . Classified as having AIDS after a series of Hep B Vaccinations . Halted all vaccinations after this as prior I had been stable , non progressive and had a normal CD4 and no VL all other labs relatively normal. Explained fatigue as ‘my aids’. But I had this all through adolescence also. Will lipid supplement therapy enhance my energy levels ?
Michael, thank you very much for your work in this field. I’m an MSc student at CNELM and had the good fortune to attend some of your brilliant lectures.
I wonder whether you have any thoughts on the relevance of raised anticardiolipin antibodies found in cfs, lupus, phospholipid syndrome with relation to this subject area. Does necrosis precipitate aps antibodies or do the antibodies cause apoptosis, and is lipid replacement therapy going to be helpful either way, or perhaps not helpful unless another more root cause is addressed?
NB I think I noticed a typo above, in paragraph 5 (ref 12) where necrosis and apoptosis seem to be transposed.
Thanks again,
Sarah
Hi Michael,
Im a bit late finding this article. Fantastic information about mitochondria and chronic conditions involving fatigue.
I am a supporter of using phospholipid to support mitchondrial function in CFS/M.E. and have read clinical trials with good results. However I do have concerns about quality of lipids in supplements. They are usually from Soy or sunflower which could have been sprayed with pesticides, GM, bleached, hexane extracted etc. I am concerned about toxins in the lipid products which could do more harm than good. What are your thoughts on quality of lipids and how to source non-toxic product for patients to use.
Thanks
Rachel
Hi Rachael, I am not able to comment on general lipid combinations as they do vary. NT factor is extracted from organic soy, that way risks of any related production chemicals are greatly minimised, windblown risks are I am afraid impossible to eliminate. The production process is proprietory but we do not see problems with chemically sensitive patients using the product. Many highly chemical sensitive people use it for energy management and do very well.
Best wishes
Michael
Hello Michael
I just had this forwarded to me by a friend.I am 57 years old and have been suffering with chronic fatigue and associated brain fog and digestive issues since 1991. While I am much better now than when I first had my whole world turned upside-down, I still am not where I want to be in terms of energy and brain performance,etc. I would love to try out this LRT, how can I get my hands on what you are describing in the article?
Thank you
Gary
Hi Gary, in the USA Allergy Research Group supply this product, and in the UK Nutri-Link does.