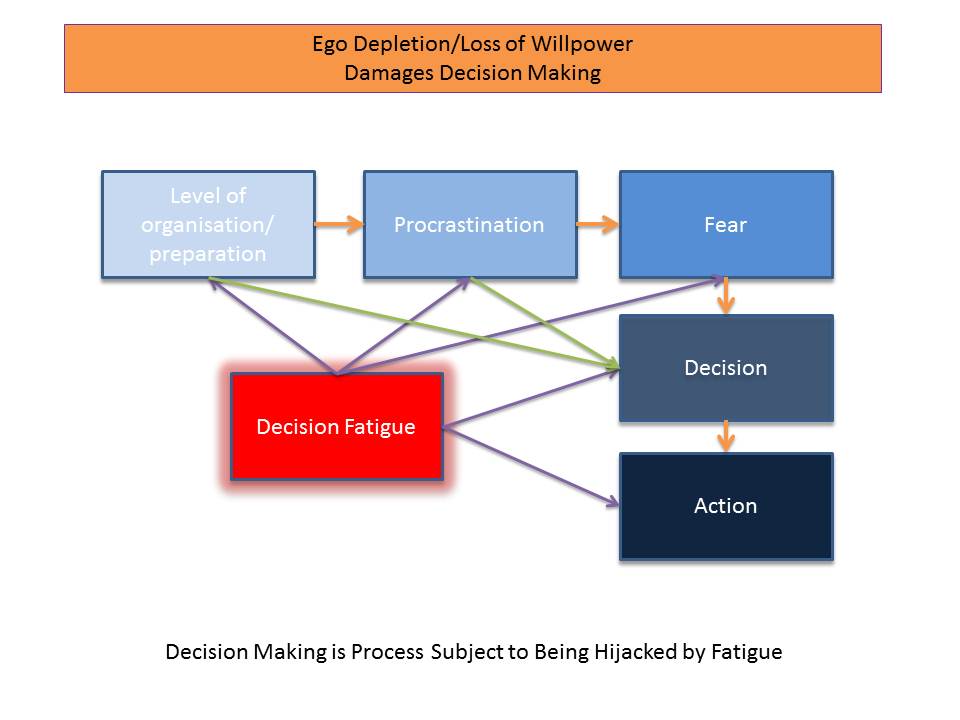
No matter how we approach decisions and how careful we are, some bad ones are made, and others are unnecessarily delayed – organisation, procrastination and fear dominate the thoughts of many paralysed by the thought of completing the decision making task.
No matter how we approach decisions and how careful we are, some bad ones are made, and others are unnecessarily delayed – organisation, procrastination and fear dominate the thoughts of many paralysed by the thought of completing the decision making task.
To complicate this further, there is the little understood effect of ‘decision fatigue’, the act of making so many decisions in a day that eventually even the best trained start to do things that in the cold light of day are difficult to justify.[1]
We pay away a biological price, a cost on our intellect as we continue throughout the days and weeks to be responsible for decisions. Whilst we may associate this with a decline in physical strength a pervasive fatigue, it is essentially a mental fatigue and accounts – so it is suggested for impulsive decisions and procrastination – the art of doing nothing.
We all know that avoiding decisions will likely bring problems later, but many people decide to put off today what will visit them tomorrow, in part this is due to the intersecting triad of organisation/preparation, procrastination and fear, but all of these are impacted upon by decision fatigue.
- Organisation/Preparation: the information you have at hand or can be acquired and the accessibility of this information to facilitate the loading of the decision making process. Lack of preparation and poor organisational skills often impede the progression of the decision.
- Procrastination: is the putting off of a decision, in part due to a perception of lack of preparation, and in part due to habits of avoiding change, or taking a decision that may carry a risk.
- Fear: is the blunt emotion that declines in the face of adequate preparations and is fuelled by procrastination and emotional constraints.
- Decision fatigue: overlays all of these elements becoming an increasingly important component of good or bad decisions as more and more decisions are made.
The result is that even highly trained individuals, once their mental energy is depleted due to increased decision making demands will make inappropriate decisions or will accede to lack of preparedness, procrastination or fear of change.
How Tiring are Decisions
It turns out that making the decision is more fatiguing than the contemplation phase or the action phase – the stage you actually progress the decision. The more decisions you have to make, the lower your reserves that you rely to make these decisions fall, leading to an increased risk of an inappropriate decision.
Fear
Part of the resistance against making decisions comes from our fear of giving up options. The word “decide” shares an etymological root with “homicide,” the Latin word “caedere,” meaning “to cut down” or “to kill,” and that loss grows in perception when decision fatigue sets in.
Once this mental depletion sets in, one of the first skills to suffer is that of compromise, and single objectives become more vital, more significant, and more easily defended. People start to drift towards their default options, as more and more decisions have to be made the desire to take the easiest option looms more and more – and at this stage having someone else make the decision for you becomes ever more attractive.
This sort of decision fatigue traps people in poor health where decisions to change behaviour can weigh heavily on them. The notion of will power at this stage is not an abstract one, the more decisions we ask a patient to make, their declining ability to make good decisions will corrupt their choices and outcomes. Income and socialisation issues further combine this into a complex mix of poor, often costly decisions in terms of their health that are then self-justified by weak arguments or repetitive statements of self-reassurance which when broken down have little substance, but in the mind of the decision fatigued individual have simply been made to preserve their mental energy at that moment, and have left them to face the cost at a later date. This deferred payment option has serious consequences, from global economics, to clinical decisions and family harmony.
Supermarkets have long understood how to target the decision fatigued consumer, placing sweets offering a quick glucose fix at the counter, when the tired shopper has already exhausted their decision making energy in the process of selecting their consumables. Their weakened resistance encourages them to make a short term decision that moves them straight to action and because long term consequences are ignored or denied it simply adds further, future problems. Problems, that will once again require decision making energy to be available for best outcomes, trapping the decision maker in a feed forward cycle of repetitive short termism, that in the context of health can drive them further and further away from the ability to maintain suitable willpower to effect a positive change.
The Brains Fuel
We all know that the brain needs a regular supply of glucose to function, and it appears that fuel also regulates willpower – if we deny the brain the fuel required to make good decisions it will increasingly make bad ones. In particular the decisions start to reflect short-term needs rather than long term planning. Immediately we can see that for those people needing to make decisions to avoid, or add in specific foods during the day, that their ability to maintain this process will be mediated by availability of suitable fuel.
This naturally throws up a classic catch 22.
- In order not to eat a person needs will power to maintain a specific nutritional choice.
- In order to have will power a person needs to eat, and selecting the best foods depend on will power.
Virtually no one has an innate gut-level sense of just how tiring it is to decide. Big decisions, small decisions, they all add up. Choosing what to have for breakfast, where to go on vacation, whom to hire, how much to spend — these all deplete willpower, and there’s no tell-tale symptom of when that willpower is low. It’s not like getting injured or hitting the wall during a marathon. Decision making energy depletion manifests itself not as one feeling but rather as a propensity to experience everything more intensely.
“Good decision making is not a trait of the person, in the sense that it’s always there, It’s a state that fluctuates.”
How Can You Deliver The Best Outcomes
If making great decisions depends on self-control, there are certain techniques that can be employed to improve this. It involves reducing the number of needless decisions that need to be made in the day:
- Plan your day so that it is not one long list of back to back events in which decisions have to be made – you can already see that clinical life is going to be a challenge here.
- Avoid regular temptations, online shopping, all you can eat buffets, discount shops etc. They all demand decision making, even it is to just to say no.
- Plan, plan and plan again – instead of making a decision every morning whether or not to exercise, or read a journal paper, schedule to do this with a colleague or have an allocated time slot. Create regular appointments so that the day becomes planned and organised – establish habits that eliminate the mental effort of making choices.
- Instead of counting on your willpower to remain robust all day, conserve it so that it’s available for important decisions and emergencies. Treat it is a valuable resource, and avoid squandering it on non-beneficial choices.
Comment
There are many situations in which the average practitioner can see that this will impact on their professional and personal life. In functional medicine, the art of telling a patients story, reflects the value of collecting relevant data in the first place and then placing into a context that they understand so that decision making then becomes a shared process.
A key elements of making a clinical decision is taking a patients social history, yet as the day wears on the desire to complete or update a patients history can be seen as one decision too many.
Taking a comprehensive social history is time-consuming. It’s easy to dismiss the task as outside your purview, especially when there’s precious little time to get through a sea of investigations and treatment options. But every patient is a person, and illness occurs in the context of multifaceted lives. We need to listen to our patients with the recognition that the most important information they can give us about their illness often lies in the folds of their social circumstances. And it’s our obligation to tailor our recommendations to that patient in their full context.
Until practitioners especially doctors understand that social history is more than a tool for passing exams, many will be practicing piecemeal medicine that leaves us all with an aroma of dissatisfaction.
Taking a good social history may be no one’s favourite decision, but it’s everyone’s responsibility.
References
[1] Baumeister RF, Bratslavsky E, Muraven M, Tice DM. Ego depletion: is the active self a limited resource? J Pers Soc Psychol. 1998 May;74(5):1252-65. View Abstract