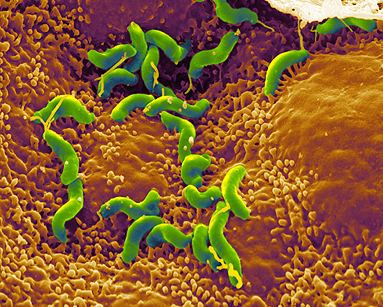
Helicobacter Pylori a Natural Approach to Eradication – Free Review
No Comments
Reading Time: 2 minutes
Dr Rachel Olivier MS ND PhD describes the pathophysiology of the infection and explores the role of natural agents in the eradication and control…