Coeliac Disease 4 Times More Common Than Previously Thought
2 Comments
Reading Time: 5 minutes
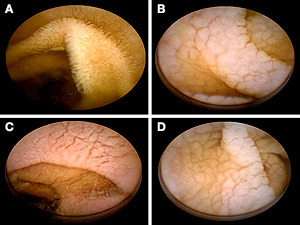
Examples of macroscopic features of villous atrophy detected by wireless capsule endoscopy in coeliac disease: A) Normal villi, B) scalloping of the mucosa on…