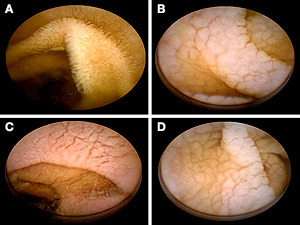
Coeliac Disease and its Many Complications
No Comments
Reading Time: 8 minutes
Coeliac disease (CD), also called gluten-sensitive enteropathy or non-tropical sprue, is a unique autoimmune disorder which results from the interaction between gluten and immune,…