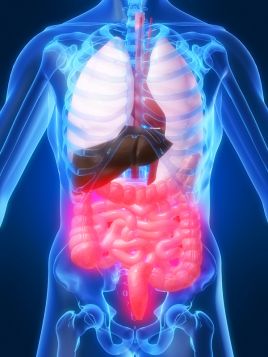
 Michael Ash BSc(Hons).DO. ND. FDipION reviews the current understanding behind bloating and distension.
Michael Ash BSc(Hons).DO. ND. FDipION reviews the current understanding behind bloating and distension.
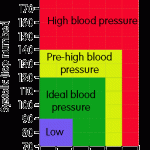
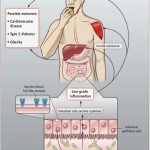
The unpleasant symptoms of bloating and abdominal distension are common and bothersome, affecting up to 96% of patients with functional gastrointestinal disorders (such as IBS) and an estimated 30% of the general population. Clear pathophysiologic explanations have been lacking and available treatment options can appear contradictory and ineffective. Treatments will be explored in a follow up review.
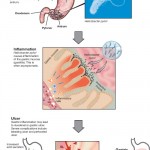
Bloating refers to the subjective sensation of abdominal swelling, whereas visible abdominal distension refers to an actual increase in abdominal girth.[1] For a long time, these have been poorly understood symptoms, but recent studies, have shed some light on the different mechanisms involved in the generation of these symptoms and summarised in this review.[2],[3]
Specialised measuring devices called abdominal inductance plethysmography (a test used to measure changes in blood flow or air volume in different parts of the body) and computed tomography ((CT) A diagnostic technique in which x-rays are taken in many different directions. A computer synthesises the x-rays to generate cross-sectional and other images of the body) have convincingly demonstrated that distension of the abdomen is a real event with some patients exhibiting as much as a 12cm increase in abdominal girth.[4]
However, bloating and distension are not always present at the same time. In IBS studies only half of ‘bloated patients’ also have visible distension.[5] This sub group of ‘bloated and distended’ patients tend to present with constipation and visceral hyposensitivity, whereas the simply ‘bloated’ group present more frequently with diahorrea and visceral hypersensitivity.
The more severe the bloating the greater the change in rectal perception[6] (The lower threshold for pain or discomfort in response to distension).[7] It may well be that bloating and distension have a mix of common and uncommon causes.
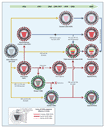
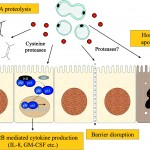
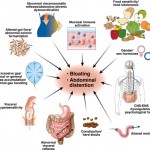
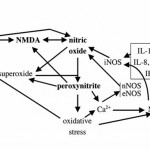
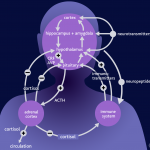
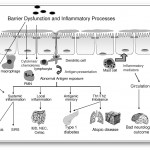
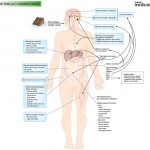
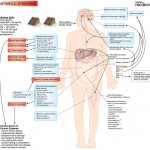
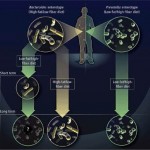
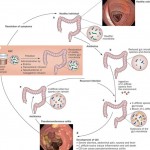
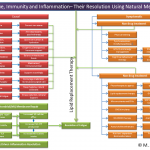
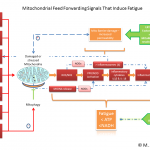
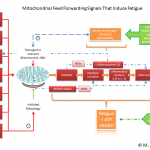
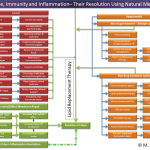
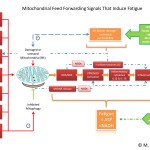
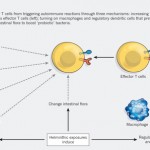
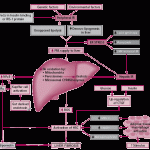
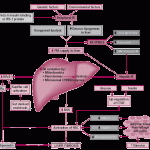
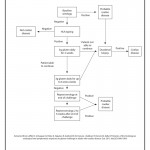
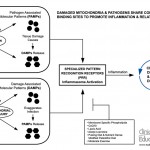
Click on the image below to see an enlarged model of possible causes and exacerbating factors in the development of bloating and distension. This diagram was extracted from: Gastroenterology. Volume 136, Issue 5, May 2009, Pages 1487-1490
Possible Explanations
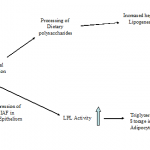
- ‘Too much gas’. Despite the immediate instinctive sense that this must be correct, detailed studies have failed to demonstrate this as a substantive cause.[8]
- Abnormal colonic fermentation has been suggested in some studies.[9]
- Defective handling of exogenous gas loads within the GI tract in patients with bloating has been convincingly identified in several studies of patients with IBS complaining of bloating. Especially in terms of transit of gas and tolerance (pain) of it.[10]
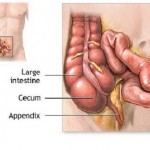
- Mechanistically, an altered GI reflex activity and enhanced sensitivity to nutrients (intolerances) have been found to be important factors involved in the impaired gas transit in these patients, as well as in symptom perception.[11],[12] These symptoms mostly emanate from the small rather than the more logical large intestine.[13]
- These studies suggest that IBS patients do not necessarily have to produce more ‘gas’ to have ‘gas-related’ symptoms, instead these may be due to motor dysfunction, producing a transport problem, and enhanced visceral sensitivity.
- Another possibility is focal gas pooling which may release abnormal viscerosomatic (a muscular response to stimulation of a nerve-receptor organ in a visceral organ) responses, resulting in bloating and visible abdominal distension.of the diaphragm.
- Excess lumbar lordosis, (forward curvature of the spine, producing a hollow in the back) weak abdominal musculature, and voluntary protrusion of the abdomen have been suggested to be of importance in the generation of bloating and abdominal distension, but none of these alterations could be confirmed by a CT study.[14]
- However, a number of other careful studies comparing healthy volunteers and patients, have provided important explanations of abdominal distension in patients with functional GI disorders. They show that abdominal accommodation to volume loads is an active process involving local muscular response and that patients with IBS and bloating have impaired viscerosomatic reflexes and abdominal wall muscular control. In patients with bloating, abdominal perception and distension in response to intra-abdominal volume increments are exaggerated markedly and associated with muscular dystony (a disorder characterised by unusual or involuntary movements or muscular spasms) of the abdominal wall.[15],[16]
- Comparing two different groups of patients with bloating revealed two different mechanisms[17]:
- Group 1: IBS patients with bloating,
- Group 2: Intestinal dysmotility (Food fails to move normally through the stomach and intestines, there often is distension of the stomach and intestines as fluid collects, and is frequently painful) and bloating.
Both sets were scanned with CT at ease and during bloating. At ease they were the same but once bloated there were differences:
- Patients with intestinal dysmotility demonstrated a true increase in total abdominal volume with upward movement of their diaphragm.
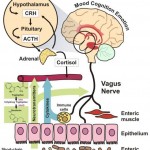
- IBS patients had a very modest increment of the abdominal volume; instead the abdominal distension was related to downward movement of the diaphragm, placing stress on the phrenic nerve (this innervates the diaphragm and controls breathing), resulting in forward (distension) redistribution of abdominal contents.[18]
Other less well-established/studied factors of potential importance are:
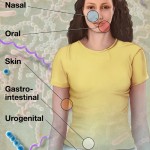
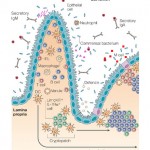
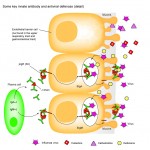
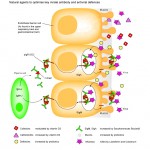
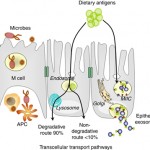
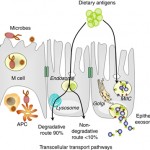
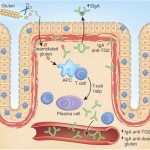
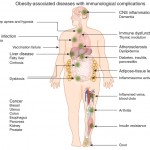
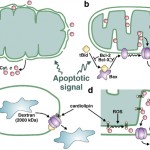
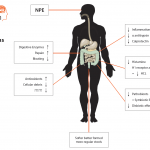
- Abnormal mucosal immune activation. A large subset of IBS patients show gender-dependent mucosal infiltration of white blood cells and histamine correlating with abdominal bloating and dysmotility-like dyspepsia (Chronic or recurrent pain in the upper abdomen) [19],[20]
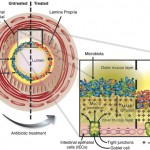
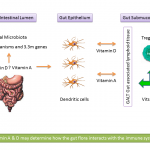
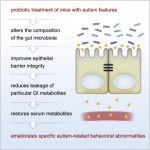
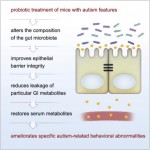
- Altered bacterial flora, investigations using sophisticated measuring techniques have revealed that the faecal flora in patients with IBS is different from healthy controls. If this is a trigger rather than a result, changing the floral balance may provide therapeutic outcomes with little risk if probiotics rather than antibiotics are used.[21],[22],[23],[24],[25]
- Sex hormones in which changes in the production of female related oestrogen and progesterone influence IBS, bloating and bowel function.[26]
- Psychological factors, including somatisation (The presence of real and significant physical symptoms that cannot be explained by a medical condition, but are instead a manifestation of anxiety or other mental distress).[27]
References
[1] Houghton LA, & Whorwell PJ (2005). Towards a better understanding of abdominal bloating and distension in functional gastrointestinal disorders. Neurogastroenterology and motility : the official journal of the European Gastrointestinal Motility Society, 17 (4), 500-11 PMID: 16078938
[2] Azpiroz F. Intestinal gas dynamics: mechanisms and clinical relevance. Gut. 2005;54:893–895. View Abstract
[3] Accarino A, Perez F, Azpiroz F, et al. Abdominal distension results from caudo-ventral redistribution of contents. Gastroenterology. 2009;136:1544–1551. View Abstract
[4] Lewis MJ, Reilly B, Houghton LA, et al. Ambulatory abdominal inductance plethysmography: towards objective assessment of abdominal distension in irritable bowel syndrome. Gut. 2001;48:216–220 View Abstract
[5] Houghton LA, Lea R, Agrawal A, et al. Relationship of abdominal bloating to distention in irritable bowel syndrome and effect of bowel habit. Gastroenterology. 2006;131:1003–1010 View Abstract
[6] Sabate JM, Veyrac M, Mion F, Siproudhis L, Ducrotte P, Zerbib F, Grimaud JC, Dapoigny M, Dyard F, Coffin B. Relationship between rectal sensitivity, symptoms intensity and quality of life in patients with irritable bowel syndrome. Aliment Pharmacol Ther. 2008 Aug 15;28(4):484-90. Epub 2008 Jun 9. View Abstract
[7] Agrawal A, Houghton LA, Lea R, et al. Bloating and distention in irritable bowel syndrome: the role of visceral sensation. Gastroenterology. 2008;134:1882–1889. View Abstract
[8] Accarino A, Perez F, Azpiroz F, et al. Intestinal gas and bloating: effect of prokinetic stimulation. Am J Gastroenterol. 2008;103:2036–2042. View Abstract
[9] King TS, Elia M, Hunter JO. Abnormal colonic fermentation in irritable bowel syndrome. Lancet. 1998;352:1187–1189. View Abstract
[10] Serra J, Azpiroz F, Malagelada JR. Impaired transit and tolerance of intestinal gas in the irritable bowel syndrome. Gut. 2001;48:14–19 View Abstract
[11] Passos MC, Serra J, Azpiroz F, et al. Impaired reflex control of intestinal gas transit in patients with abdominal bloating. Gut. 2005;54:344–348. View Abstract
[12] Simrén M, Abrahamsson H, Björnsson ES. An exaggerated sensory component of the gastrocolonic response in patients with irritable bowel syndrome. Gut. 2001;48:20–27. View Abstract
[13] Salvioli B, Serra J, Azpiroz F, et al. Impaired small bowel gas propulsion in patients with bloating during intestinal lipid infusion. Am J Gastroenterol. 2006;101:1853–1857. View Abstract
[14] Maxton DG, Martin DF, Whorwell PJ, et al. Abdominal distension in female patients with irritable bowel syndrome: exploration of possible mechanisms. Gut. 1991;32:662–664 View Abstract
[15] Villoria A, Azpiroz F, Soldevilla A, et al. Abdominal accommodation: a coordinated adaptation of the abdominal wall to its content. Am J Gastroenterol. 2008;103:2807–2815. View Abstract
[16] Tremolaterra F, Villoria A, Azpiroz F, et al. Impaired viscerosomatic reflexes and abdominal-wall dystony associated with bloating. Gastroenterology. 2006;130:1062–1068. View Abstract
[18] Perez F, Accarino A, Azpiroz F, et al. Gas distribution within the human gut: effect of meals. Am J Gastroenterol. 2007;102:842–849. View Abstract
[19] Cremon C, Gargano L, Morselli-Labate AM, Santini D, Cogliandro RF, De Giorgio R, Stanghellini V, Corinaldesi R, & Barbara G (2009). Mucosal immune activation in irritable bowel syndrome: gender-dependence and association with digestive symptoms. The American journal of gastroenterology, 104 (2), 392-400 PMID: 19174797
[20] Barbara G, Stanghellini V, De Giorgio R, Cremon C, Cottrell GS, Santini D,Pasquinelli G, Morselli-Labate AM, Grady EF, Bunnett NW, Collins SM, Corinaldesi,R. Activated mast cells in proximity to colonic nerves correlate with abdominal pain in irritable bowel syndrome. Gastroenterology. 2004 Mar;126(3):693-702. View Abstract
[21] Kassinen A, Krogius-Kurikka L, Makivuokko H, et al. The fecal microbiota of irritable bowel syndrome patients differs significantly from that of healthy subjects. Gastroenterology. 2007;133:24–33. View Abstract
[22] Posserud I, Stotzer PO, Bjornsson ES, et al. Small intestinal bacterial overgrowth in patients with irritable bowel syndrome. Gut. 2007;56:802–808. View Abstract
[23] Quigley EM The efficacy of probiotics in IBS. J Clin Gastroenterol. 2008 Jul;42 Suppl 2:S85-90. View Abstract
[24] Quigley EM. Probiotics in irritable bowel syndrome: an immunomodulatory strategy?J Am Coll Nutr. 2007 Dec;26(6):684S-90S. View Abstract
[25] Agrawal A, Houghton LA, Morris J, et al. Clinical trial: the effects of a fermented milk product containing Bifidobacterium lactis DN-173-010 on abdominal distension and gastrointestinal transit in irritable bowel syndrome with constipation. Aliment Pharmacol Ther. 2008;Sep 17
[26] Jiang X, Locke GR, Choung RS, et al. Prevalence and risk factors for abdominal bloating and visible distention: a population-based study. Gut. 2008;57:756–763 View Abstract
[27] Chang L, Lee OY, Naliboff B, et al. Sensation of bloating and visible abdominal distension in patients with irritable bowel syndrome. Am J Gastroenterol. 2001;96:3341–3347. View Abstract















































































































































































































































































































































































































































































































































































































































































































































































3 Comments. Leave new
Really interesting article, fascinating to start looking a various underlying factors involved in bloating and distention. Looking forward to the follow up with treatment implications. Will you also cover diagnosis? For example how would different factors that lead to bloating or distension show up on a stool test?
Many Thanks
Ange
Can you recommend a nutritional protocol for someone with constant abdominal distension – is there anything that can help with this?
Dear Sarah
There are a number of individual causes of bloating, and of course many of these will coexist requiring a careful elucidation of causal as well as correlative triggers.
A qualified nutritional therapist should be able to provide a structured approach to this condition, resulting in a treatment recommendation.
The key areas they may assess will be dietary choice, and potential reactivity as well as investigational work ups, these may include immunology as well as microbiological investigations and digestive function tests as well as discussion of lifestyle and persoal history in case there is any psychosomatic involvement as well as the triggers discussed.
The list in the article is comprehensive but not exhaustive. I will be reviewing investigations and treatment options in the next few weeks. In the meantime please call Nutri-Link Ltd (08450 760 402) who may be able to recommend a Nutritional Therapist near to you.
Michael