 Vitamin D is increasingly understood to be an essential component of many aspects of human health and although technically not a “vitamin,” vitamin D is in a class by itself. Its metabolic product, calcitriol, is actually a secosteroid (A compound derived from a steroid in which there has been a ring cleavage) hormone that binds to over 2000 gene receptors (about 10% of the human genome) in the human body. There are 3 recognised ways for adults to ensure adequate levels of vitamin D:
Vitamin D is increasingly understood to be an essential component of many aspects of human health and although technically not a “vitamin,” vitamin D is in a class by itself. Its metabolic product, calcitriol, is actually a secosteroid (A compound derived from a steroid in which there has been a ring cleavage) hormone that binds to over 2000 gene receptors (about 10% of the human genome) in the human body. There are 3 recognised ways for adults to ensure adequate levels of vitamin D:
These are:
- Regularly receive midday sun exposure in the late spring, summer, and early autumn, exposing as much of the skin as possible but at least 25% (being careful to never burn).
- Regularly use a sun bed (avoiding sunburn) during the darker seasons.
- Take 5,000 IU vitamin D 3 supplementation per day for 2–3 months, then obtain a 25-hydroxyvitamin D test. Adjust your dosage so that blood levels are between the currently recommended 50–80 ng/mL (or 125–200 nM/L) year-round.
If healthy adults and adolescents regularly avoid sunlight exposure, research indicates a necessity to supplement with at least 5,000 units (IU) of vitamin D daily.[1],[2],[3] To obtain this amount from milk alone they would need to consume at least 50 glasses. With a multivitamin more than 10 tablets would be necessary. Neither is advisable. Specialised supplementation is recommended including the use of research supported supplements as provided by Biotics Research Corportaion taken at the correct time to ensure optimal absorption.
Vitamin D refers to two biologically inactive precursors – D3, also known as cholecalciferol, and D2, also known as ergocalciferol. Both D3 and D2 precursors are hydroxylated in the liver and kidneys to form 25- hydroxyvitamin D (25(OH)D), the non-active ‘storage’ form, and 1,25-dihydroxyvitamin D (1,25(OH)2D), the biologically active form that is tightly controlled by the body.
Questions have also been raised as to whether the pursuit of vitamin D from sunlight exposure places the person at risk of any skin irritation/damage that may negate the benefits gained from the vitamin D production. This article out in the journal of dermatology this June 2010, suggests that supplementation is the safest route to optimal supplementation and keeps the risk of skin related damage and cancer formation to a minimum.[4]
An ever growing body of science supports the benefits of maintaining healthy vitamin D levels. In adults, it is said vitamin D deficiency may precipitate or exacerbate osteopenia, osteoporosis, muscle weakness, fractures, common cancers, autoimmune diseases, infectious diseases and cardiovascular diseases. There is also some evidence that the vitamin may reduce the incidence of several types of cancer and type-1 diabetes.
The skin produces approximately 10,000 IU vitamin D in response 20–30 minutes summer sun exposure—50 times more than the UK’s government’s recommendation of 200 IU per day! The researchers go on to say:
Because of these practical difficulties combined with the detrimental side effects of UV exposure, we endorse the IARC assessment that even if it is ultimately demonstrated that increasing vitamin D levels impacts cancer and chronic disease, oral supplements of vitamin D would probably represent the safest way to increase vitamin D status.
Comment
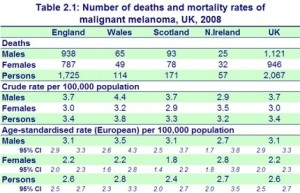
As one might expect the dermatology orientated physicians remain concerned that over, or unsuitable exposure to UV light increases the risk of skin cancers and wish to continue to support their long term conservative message to keep covered up. The incidence of death related to vitamin D insufficiency globally has been estimated at in excess of 600,000 preventable deaths per year.[5] In the UK about 2,500 die from skin cancer each year, and what is not really understood is that melanoma, the most deadly of the cancers mostly occur on the non sun exposed parts of the skin, and that incidence of melanoma declines with appropriate sunlight exposure, due to the benefits derived from vitamin D production.[6]
Here remains the conflict as sensible sunbathing or sun exposure is beneficial and this requires no sun block, but non sensible sunbathing is clearly a risk. Those of us living in the northern hemisphere really only have to consider the risks of over exposure on a rare few days, and the risk of vitamin D deficiency is far higher due to the limited amount of sun during 6 months of the year.
References
[1] Vieth R. Experimentally observed vitamin D requirements are higher than extrapolated ones. Am J Clin Nutr. 2009 Oct;90(4):1114-5; author reply 1115-6. Epub 2009 Aug 26
[2] Yetley EA, Brulé D, Cheney MC, Davis CD, Esslinger KA, Fischer PW, Friedl KE, Greene-Finestone LS, Guenther PM, Klurfeld DM, L’Abbe MR, McMurry KY, Starke-Reed PE, Trumbo PR. Dietary reference intakes for vitamin D: justification for a review of the 1997 values. Am J Clin Nutr. 2009 Mar;89(3):719-27. Epub 2009 Jan 28. View Full Paper
[3] Chung M, Balk EM, Ip S, Lee J, Terasawa T, Raman G, Trikalinos T, Lichtenstein AH, Lau J. Systematic review to support the development of nutrient reference intake values: challenges and solutions. Am J Clin Nutr. 2010 May 26. View Abstract
[4] Terushkin V, Bender A, Psaty EL, Engelsen O, Wang SQ, Halpern AC. Estimated equivalency of vitamin D production from natural sun exposure versus oral vitamin D supplementation across seasons at two US latitudes. J Am Acad Dermatol. 2010 Jun;62(6):929.e1-9. Epub 2010 Apr 3 View Abstract
[5] Garland CF, Gorham ED, Mohr SB, Grant WB, Giovannucci EL, Lipkin M, Newmark H, Holick MF, Garland FC. Vitamin D and prevention of breast cancer: pooled analysis. J Steroid Biochem Mol Biol. 2007 Mar;103(3-5):708-11. View Abstract
[6] Holick MF. Sunlight, UV-radiation, vitamin D and skin cancer: how much sunlight do we need? Adv Exp Med Biol. 2008;624:1-15. Review. View Abstract





