 A recent Cochrane review suggests that diabetic patients should keep to a low salt diet to prevent diabetic kidney disease. Their collaboration review looked at 13 studies. These included 254 patients suffering from type 1 and type 11 diabetes and noted that reducing salt intake by a whopping 8.5mg per day matched the effects experienced from a single antihypertensive medication (7.1/3.1 mmHg – type 1, 6.9/2.9 mmHg type 11).[1] They also acknowledged that this was a short study – so the effect was noticed in just 7 days, but that it would be difficult to maintain over a longer period.
A recent Cochrane review suggests that diabetic patients should keep to a low salt diet to prevent diabetic kidney disease. Their collaboration review looked at 13 studies. These included 254 patients suffering from type 1 and type 11 diabetes and noted that reducing salt intake by a whopping 8.5mg per day matched the effects experienced from a single antihypertensive medication (7.1/3.1 mmHg – type 1, 6.9/2.9 mmHg type 11).[1] They also acknowledged that this was a short study – so the effect was noticed in just 7 days, but that it would be difficult to maintain over a longer period.
High sodium intake (>2500mg per day) is recognised by health authorities the world over as a reliable (if not controversial) predictor of hastened mortality and risk of coronary heart disease, independent of other cardiovascular risk factors, including blood pressure. This relationship has been measured using urinary output as a risk identifier and the results from these tests provide direct evidence of the harmful effects of high salt/sodium intake in the adult population.[2] High sodium intake may also be associated with higher rates of stomach cancer, asthma disorders and infections.
All well and good but excluding sodium from the diet in the UK – a policy well established over the last few years (since 2003)and taken on board by many food manufacturers appears to have simply increased the amount of salt added at the table. The FSA have trumpeted their campaign as a success and have declared an average reduction in salt consumption from 9.5gm per day in 2003 to 8.6gm in 2008 – but are they missing the point.
Salt reduction alone – or at least sodium chloride reduction has a less than convincing series of statistical data sets to suggest this is the panacea of cardiovascular mortality reduction.3
Patients and members of the public are more salt aware, but slow to adopt changes, in part this is because of the dietary sources of salt and the other is taste or a perception of taste that has reduced the uptake of UK available lower sodium alternatives.[3]

However, in Europe we have one long term study that on closer investigation suggests that a population wide approach to sodium reduction and mineral supplementation over 30 years has made a significant contribution that that countries cardiovascular disease incidence.
Finnish Experiences
Finland, a country that uses a regulatory approach, provides one of the best examples of population reductions in sodium intake. Since the early 1970s, Finland has had a population-based policy for sodium reduction anchored on partnership and regulation of the food industry and consumer education via mass media.
In Finland, cross-sectional population surveys to monitor cardiovascular risk factors have been carried out since the 1970’s. This is in line with the Finnish Governments health policy to reduce total sodium intake by changing their salt in food production and flavouring to mineral enriched salt substitutes. In Finland even McDonalds uses this salt. This is recognised to reduce the risk of sodium related disease as the competing minerals, potassium and magnesium increase sodium excretion, and l-lysine improves taste and aids in vascular flexibility.
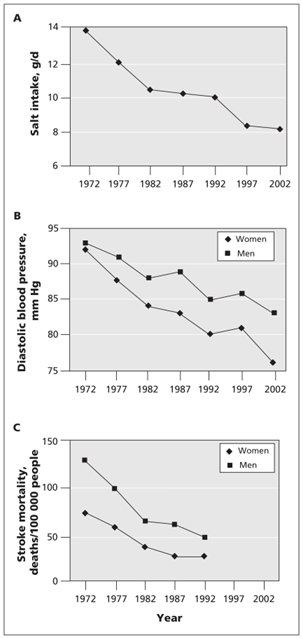
Between 1979 and 2002 urinary sodium excretion in Finland decreased from over 220 to less than 170 mmol/day among men and from nearly 180 to less than 130 mmol/day among women. Although potassium excretion decreased somewhat as well, the decrease in sodium-potassium molar ratio was also significant. Annual cardiovascular mortality has decreased by about 80% since the 1970s, a further decrease in sodium intake however, still remains a goal for the Finnish food industry and consumers.[4]
The indication here is that sodium reduction alone does not account for the dramatic improvements in CVD, but that the supportive nutrients (potassium/magnesium/calcium) have also played an important part. As mentioned earlier a paper published in 2007 reviewing over 400 papers also suggests that sodium reduction alone is inadequate as a mechanism for significant CVD reduction.[5] This paper has, as one might imagine been embraced by the Salt Association as a means of validating continued use of pure dried vacuum (PDV) salt (NaCl) in food production.[6]
Scientists in Finland said in explanation:
…In fact, 85 to 90 percent of this dramatic reduction in deaths is due entirely to simple diet changes; reduction of saturated/unsaturated fat ratio and, according to the study on this phenomenon, a nationwide “…replacement of common salt by a novel sodium-reduced, potassium, magnesium-, and l-lysine HCI-enriched salt, both in home kitchens and in the food industry.”[7]
The paper went on to note that during the same time period
“…marked increases in the intake of alcohol, obesity among men, and smoking among women have been observed.”
The lead scientist’s in further analysis state:
During the past 30 years, the one-third decrease in the average salt intake has been accompanied by a more than 10-mm Hg fall in the population average of both systolic and diastolic blood pressure, and a 75% to 80% decrease in both stroke and coronary heart disease mortality in Finland……….. with an increase in life expectancy of both male and female Finns of six to seven years.[8]
There is convincing evidence, which indicates that this imbalance, that is, the high intake of sodium on one hand and the low intakes of potassium, calcium, and magnesium on the other hand associated with high intake of NaCl, produce and maintain elevated blood pressure in a big proportion of the population. Decreased intakes of sodium, and increased intakes of potassium, calcium, and magnesium each alone, decrease elevated blood pressure.
So -a combination of all these factors, that is, decrease of sodium and increase of potassium, calcium, and magnesium intakes, characteristic of the so-called Dietary Approaches to Stop Hypertension diets (DASH), have an excellent blood pressure lowering effect.
UK Position
Most people in the UK eat much more salt/sodium than they should. On average the general public are eating 9.5g salt (about 3.7g sodium) a day, many of course eat much more, but we should be consuming no more than 6 g salt (2.4g sodium). Processed foods top the list for sodium contribution in both the United States and the United Kingdom and are estimated to account for over 70% of sodium intake.[9]
Reducing salt intake by around 2.5g a day diminishes our risk of having a stroke or heart attack by one quarter. As a population, for each gram of salt that UK individuals cut out of the national average intake, will save over 6,500 lives each year. It will also prevent over 6,500 heart attacks and strokes each year.[10] Reducing salt is one of the quickest ways to reduce your blood pressure, particularly if you already have high blood pressure.[11]
The Committee on Medical Aspects of Food Policy (COMA) recommended a reduction in the average intake of NaCl from food by the adult population from the current level of 9000 mg/day (150 mmol/day) to 6000 mg/day (100 mmol/day) (COMA, 1994[12]).[13]
Simulations in the USA even suggest that achieving a salt reduction of 3 g/day in the American diet (approximately 29% of daily intake for men and 41% for women) could benefit public health more than targeting tobacco, weight loss or cholesterol levels, and prevent as many deaths as antihypertensive drugs would prevent if given to everyone with hypertension.[14]
Industrialised countries average an intake of 3,000-4,500mg of sodium per day against an RDI of 1,500mg. This means that to obtain the benefits from sodium reduction alone, total intake would have to be reduced to 300-450mg per day from all sources.
Or replacement with the Finish low sodium mineral enriched salt substitute at 3,000-4,500 appears to achieve the same effect due to the increased amounts of magnesium and potassium and lysine Hcl.[15]
In the UK company called Klinge Foods product -LoSalt holds 50%-70% of the UK market share in low sodium/high potassium salt substitutes based on Nielsen figures of April 2010. It also supplies its product to a total of 30 different countries and is still the UK’s only specialised producer of potassium chloride.[16]
This product whilst not the subject of 30 years of research offers the UK consumer a suitable alternative to NaCl (table salt) and provides an acceptable taste substitute.
Comparisons
The Finnish mineral salt is a salt replacement product made with a patented blend of sodium chloride, potassium chloride, magnesium sulphate[17] and lysine hydrochloride. lysine is a building block of the amino acid carnitine, which has been shown to help heal and strengthen arterial walls by using the lysine binding sites on the side of arterial walls to facilitate dilation and pressure reduction as well as contributing to taste enhancement.
Product Comparison Chart
| LoSalt | Finnish Salt |
Common Salt | |||
| NaCl: | 33.3% (Sodium Chloride) | NaCl: | 56%(Sodium Chloride) | NaCl: | 98 – 100% (Sodium Chloride) |
| KCI | 66.6% (Potassium Chloride) | KCI | 28%(Potassium Chloride) | ||
| I-lysine-HCI | 2%, | ||||
| MgSO4.7H2O | 12% (Magnesium Sulphate Heptahydrate) | ||||
| Iodine if reqd | (25mg/kg) | ||||
| Anti caking agent | .1% (Magnesium Carbonate) | Anti caking agent | 2%(Silicon Dioxide) | ||
Salt Sensitivity
The need for reduced sodium intake is even higher in genetically sensitised individuals. In a normo-tensive population (320 subjects) approximately 30% were shown to be salt-sensitive, irrespective of ethnic origin. Characteristics shared by ‘salt-sensitive’ individuals include differences in responses of the renin-angiotensin and sympathetic nervous systems, renal function, body fat distribution, insulin resistance and intracellular ion transport.10
If a person wishes to decrease his/her blood pressure using just a low-sodium-diet he/she needs to reduce the intake of normal salt to 10% if he/she wishes to get the same effect on blood pressure as switching to the equivalent to the Mineral rich Finnish salt in line withe DASH strategy; i.e. taking relevant mineral enriched salts is 9 x more effective than sodium exclusion alone.[18],[19]. Potassium[20], magnesium[21] and lysine intensify the excretion of sodium in the human body and supports patients on hypertensive medication suggesting considerable safety.[22]
Of course, sodium isn’t all bad. It’s critical for proper functioning of the body. Sodium is important for proper nerve conduction, allows certain nutrients to go in and out of cells, assists in maintaining optimal blood pressure and is necessary for controlling fluid levels. Moderation, though, is key.
Dairy, meat, poultry, fish, and vegetables naturally contain sodium, and canned vegetables, soups, deli or lunch meats, processed cheese, savoury snacks and frozen foods can contain upwards of 1,000 mg of sodium per serving. So it’s easy to consume excess sodium, even when you’re trying to cut back. According to the McDonald’s Nutrition Chart, one Big Mac contains 1040 mg (or 1.04 grams) of sodium other products of theirs include up to 2070mg per meal![23]
Cautionary Notes
Potassium rich salts have to be cautiously used in people with diabetes and kidney disease. High potassium levels, or hyperkalemia, has two causes.
- It can be caused by the body getting too much potassium, in food or medication, or
- the body releasing too much potassium into the blood stream.
There are often no symptoms of high potassium levels, especially in milder cases.
There are several reasons why blood cells may give up their potassium. When there is tissue trauma, such as burning, gastrointestinal bleeding, surgery, traumatic injury, or rhabdomyolysis, cells will release potassium into the blood stream. In most cases, tissue trauma isn’t sufficient to cause high potassium levels on its own. Usually there is poor kidney function, a shortage of the hormone aldosterone, or increased potassium intake in addition to tissue trauma. Some medications, salt replacements, and low sodium foods are especially high in potassium and should be monitored if there is a risk for high potassium levels in a patient’s blood stream. Heart failure is the critical end point in patients unable to excrete potassium.
Comment
The role of sodium in elevating blood pressure and increasing the risk for other lifestyle diseases is considered to be well understood, but remains controversial. The idea of simply following a sodium exclusion diet is less clear in terms of outcome and hard to apply on a national policy basis. The inclusion of additional minerals as demonstrated by the Finnish experience adds considerable benefit to the gain in quality of life outcomes and appears to meet the taste complications as well. In the UK we have a low sodium potassium rich substitute which does not have the same level of research as the Finnish experience but does support collective opinion. If the risk of increasing potassium alone exists – it does so in a subset of patients, all of whom would receive appropriate recommendations concerning potassium intake from their primary care provider.
We as nutritional therapists recognise tat changing peoples habits are hard, and that the easier this can be made the better, salt reduction needs to go hand in hand with taste and ease of access as well as demonstrable benefits to be sure the consumer makes his or her correct choice at the till.
References
[1] Suckling RJ, He FJ, MacGregor GA. Altered dietary salt intake for preventing and treating diabetic kidney disease. Cochrane Database of Systematic Reviews 2010, Issue 12. Art. No.: CD006763. DOI: 10.1002/14651858.CD006763.pub2 View Article
[2] Tuomilehto J, Jousilahti P, Rastenyte D, Moltchanov V, Tanskanen A, Pietinen P, Nissinen A. Urinary sodium excretion and cardiovascular mortality in Finland: a prospective study. Lancet. 2001 Mar 17;357(9259):848-51. View Abstract
[3] Hayes JE, Sullivan BS, Duffy VB. Explaining variability in sodium intake through oral sensory phenotype, salt sensation and liking. Physiol Behav. 2010 Jun 16;100(4):369-80. Epub 2010 Apr 7. View Abstract
[4] Laatikainen T, Pietinen P, Valsta L, Sundvall J, Reinivuo H, Tuomilehto J. Sodium in the Finnish diet: 20-year trends in urinary sodium excretion among the adult population. Eur J Clin Nutr. 2006 Aug;60(8):965-70. Epub 2006 Feb 15. View Abstract
[5] Walker J, MacKenzie AD, Dunning J. Does reducing your salt intake make you live longer? Interact Cardiovasc Thorac Surg. 2007 Dec;6(6):793-8. Epub 2007 Sep 2. View Full Paper
[6] http://www.saltsense.co.uk/
[7] Karppanen H, Mervaala E. Adherence to and population impact of non-pharmacological and pharmacological antihypertensive therapy. J Hum Hypertens. 1996 Feb;10 Suppl 1:S57-61. View Abstract
[8] Karppanen H, Mervaala E. Sodium intake and hypertension. Prog Cardiovasc Dis. 2006 Sep-Oct;49(2):59-75. Review. View Abstract
[9] Mattes RD, Donnelly D. Relative contributions of dietary sodium sources. J Am Coll Nutr 1991;10:383–93 View Abstract
[10] Consensus Action on Salt and Health Web Site View Page
[11] He FJ & MacGregor GA. Effect of modest salt reduction on blood pressure: a meta-analysis of randomized trials. Implications for public health. Journal of Human Hypertension. 2002; 16, 761-770 View Abstract
[12] COMA (1994). Nutritional Aspects of Cardiovascular Disease. Report of the Cardiovascular Review Group, Committee on Medical Aspects of Food and Nutrition Policy. HMSO, London.
[13] EVM Review of Sodium Cloride. View PDF
[14] Bibbins-Domingo K, Chertow GM, Coxson PG, et al. Projected effect of dietary salt reductions on future cardiovascular disease. N Engl J Med 2010;362:590–9. View Abstract
[15] Karppanen H, Karppanen P, Mervaala E. Why and how to implement sodium, potassium, calcium, and magnesium changes in food items and diets? J Hum Hypertens. 2005 Dec;19 Suppl 3:S10-9. Review. View Abstract
[16] Klinge Foods Web Site: http://www.klinge-chemicals.co.uk/
[17] Ueshima K. Magnesium and ischemic heart disease: a review of epidemiological, experimental, and clinical evidences. Magnes Res. 2005 Dec;18(4):275-84. Review. View Abstract
[18] Karppanen H, Marvaala E 2006 Progress in Cardiovascular diseases vol 49, No. 2 (Sep-Oct) 2006, 59-75
[19] Karppanen H, Tanskanen A, Tuomilehto J, Puska P, Vuori J, Jäntti V, Seppänen ML. Safety and effects of potassium- and magnesium-containing low sodium salt mixtures. J Cardiovasc Pharmacol. 1984;6 Suppl 1:S236-43. View Abstract
[20] He FJ, MacGregor GA. Beneficial effects of potassium on human health. Physiol Plant. 2008 Aug;133(4):725-35. Review. View Abstract
[21] Saris NE, Mervaala E, Karppanen H, Khawaja JA, Lewenstam A. Magnesium. An update on physiological, clinical and analytical aspects. Clin Chim Acta. 2000 Apr;294(1-2):1-26. Review. View Abstract
[22] Mervaala EM, Paakkari I, Laakso J, Nevala R, Teräväinen TM, Fyhrquist F, Vapaatalo H, Karppanen H. Replacement of salt by a novel potassium- and magnesium-enriched salt alternative improves the cardiovascular effects of ramipril. Br J Pharmacol. 1994 Apr;111(4):1189-97. View Abstract






2 Comments. Leave new
Hi
There are other salt products on the UK market that offer reduction in sodium. MILLDOWN salt offers 66.7% reduction in sodium and is suitable for use in a salt grinder. It has no flowing agents or hidden flowing agents, More info on http://www.milldownsalt.com. It has the same flavour as sea salt
The reduction in overall sodium content is something to be regarded as being helpful in terms of total sodium intake. The difference between reduced sodium and mineral enriched salts is in the change of vascular pressure experienced in both animal and human models. The combination of magnesium, potassium and L-Lysine confers a greater impact on human health than reduction of sodium alone, albeit that teste is driver in peoples decision to add or reduce intake, the mineral enriched salt confers a greater beneit the more that is consumed, whereas even in sodium reduced salt the inverse will be the outcome.